Session:: ePosters-Mon1015-M7: Benign Abdominal
EP845 - Necrotizing Soft Tissue Infection Following Percutaneous Drainage of a Diverticular Abscess: A Complex Course of Recurrent Complicated Diverticulitis
Monday, May 11, 2026
10:47 AM - 10:52 AM ET

Madeline J. Sebastian, MD
Resident Physician
DMC Sinai Grace Hospital
Royal Oak, Michigan, United StatesDisclosure information not submitted.
ePoster Presenter(s)
Purpose/Background: Percutaneous drainage is a mainstay in the management of diverticular abscesses, offering a minimally invasive alternative to urgent surgery. Although generally safe, rare but life-threatening complications such as necrotizing soft tissue infection (NSTI) can occur along the drainage tract. We present a case of NSTI following percutaneous drainage of a diverticular abscess in a patient with recurrent complicated diverticulitis, highlighting diagnostic challenges and the importance of early surgical intervention.
Methods/Interventions: A 36-year-old woman with a history of endometrial cancer status post hysterectomy, recurrent complicated diverticulitis, and obesity presented with severe left lower quadrant pain. CT imaging revealed a recurrent diverticular abscess, for which she underwent CT-guided percutaneous drainage. Cultures grew Escherichia coli, Morganella morganii, Enterococcus faecalis, and MRSA, and she was initiated on broad-spectrum intravenous antibiotics. Despite initial improvement, she developed recurrent fever, leukocytosis, and progressive tenderness at the drain site. Repeat imaging demonstrated subcutaneous emphysema along the catheter tract suspicious for NSTI. She underwent emergent incision and drainage with extensive debridement of necrotic abdominal wall tissue; intraoperative findings confirmed necrotizing infection tracking from the percutaneous drain site. Wound and tissue cultures again grew mixed enteric flora. Postoperatively, she required prolonged wound care, total parenteral nutrition, and intravenous antibiotics. A persistent colocutaneous fistula later developed at the previous drain site.
After nutritional and clinical optimization, the patient underwent elective robotic-assisted sigmoid colectomy with primary anastomosis and takedown of the colocutaneous fistula. Dense inflammatory adhesions involving the sigmoid colon and abdominal wall were encountered but successfully managed laparoscopically.
Results/Outcomes: The patient tolerated definitive robotic sigmoid colectomy well without intra-operative complications. Postoperatively, her inflammatory markers normalized, and wound healing progressed appropriately. She transitioned from parenteral to oral nutrition, completed her antibiotic course, and was discharged home in stable condition.
Conclusion/Discussion: NSTI developing after percutaneous drainage of a diverticular abscess is rare but potentially fatal. Early recognition of disproportionate pain, soft tissue emphysema, or systemic toxicity in the presence of a drain should prompt immediate surgical evaluation. This case underscores the need for vigilance in post-procedural monitoring and highlights the critical role of timely surgical debridement and multidisciplinary management in optimizing outcomes. These principles are especially true in morbidly obese patients in which the percutaneous drain courses across more subcutaneous fat, leaving the tract highly susceptible to soft tissue infection.
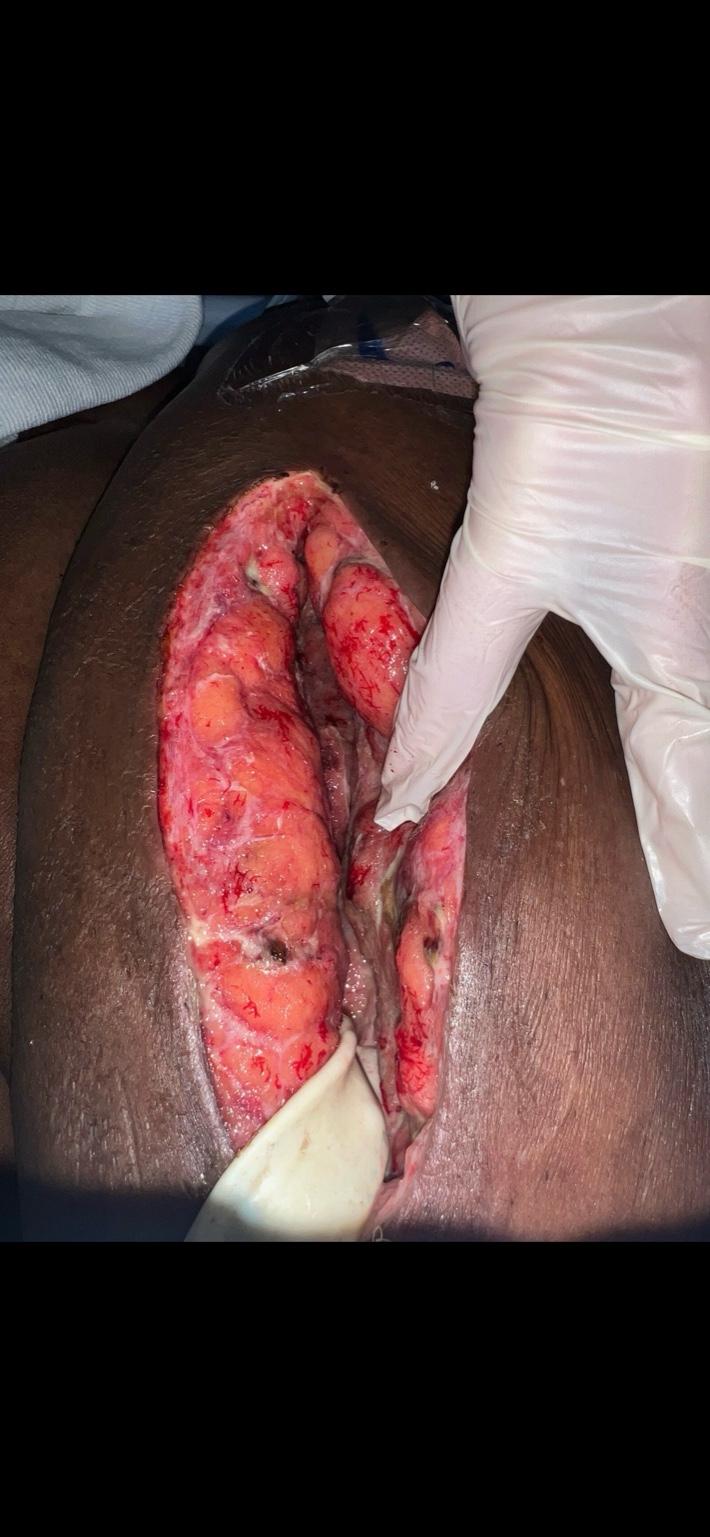
Few days status post abdominal wall debridement
Methods/Interventions: A 36-year-old woman with a history of endometrial cancer status post hysterectomy, recurrent complicated diverticulitis, and obesity presented with severe left lower quadrant pain. CT imaging revealed a recurrent diverticular abscess, for which she underwent CT-guided percutaneous drainage. Cultures grew Escherichia coli, Morganella morganii, Enterococcus faecalis, and MRSA, and she was initiated on broad-spectrum intravenous antibiotics. Despite initial improvement, she developed recurrent fever, leukocytosis, and progressive tenderness at the drain site. Repeat imaging demonstrated subcutaneous emphysema along the catheter tract suspicious for NSTI. She underwent emergent incision and drainage with extensive debridement of necrotic abdominal wall tissue; intraoperative findings confirmed necrotizing infection tracking from the percutaneous drain site. Wound and tissue cultures again grew mixed enteric flora. Postoperatively, she required prolonged wound care, total parenteral nutrition, and intravenous antibiotics. A persistent colocutaneous fistula later developed at the previous drain site.
After nutritional and clinical optimization, the patient underwent elective robotic-assisted sigmoid colectomy with primary anastomosis and takedown of the colocutaneous fistula. Dense inflammatory adhesions involving the sigmoid colon and abdominal wall were encountered but successfully managed laparoscopically.
Results/Outcomes: The patient tolerated definitive robotic sigmoid colectomy well without intra-operative complications. Postoperatively, her inflammatory markers normalized, and wound healing progressed appropriately. She transitioned from parenteral to oral nutrition, completed her antibiotic course, and was discharged home in stable condition.
Conclusion/Discussion: NSTI developing after percutaneous drainage of a diverticular abscess is rare but potentially fatal. Early recognition of disproportionate pain, soft tissue emphysema, or systemic toxicity in the presence of a drain should prompt immediate surgical evaluation. This case underscores the need for vigilance in post-procedural monitoring and highlights the critical role of timely surgical debridement and multidisciplinary management in optimizing outcomes. These principles are especially true in morbidly obese patients in which the percutaneous drain courses across more subcutaneous fat, leaving the tract highly susceptible to soft tissue infection.
Few days status post abdominal wall debridement

